Meet Dr. Pugh We are excited to welcome Dr. Thomas Pugh to Anova Cancer Care. He is a Radiation Oncologist who specializes in the use of radiation
Read MoreUrology Associates Blog
Dr. Jordan Alger Offers Aquablation Therapy at Urology Associates
Denver's CBS4, recently interviewed Dr. Jordan Alger and one of his patients who underwent the new Aquablation procedure. Aquablation is a new,
Read MoreNew Research Shows Cyberknife Therapy Is More Effective Than Conventional Radiation
Patients who underwent treatment with Cyberknife demonstrated a 5-year disease control rate of 96%, compared with 95% among patients who underwent
Read MoreBig News for Individuals Who Need Insurance Coverage for Fertility.
On April 13, 2022, Governor Polis signed into law HB22-1008 on Implementation of Fertility Coverage. In 2020, Colorado passed HB20-1158 Colorado
Read MoreUrology Associates Has Partnered With Urology America
We are excited to announce a new partnership with Urology America, based out of Austin, Texas. We looking forward to great things ahead for
Read MorePeeing During Sex is Very Common – Is it Urination or Orgasm?
Peeing during sex is very common. Approximately 60% of women with urinary incontinence leak during sex. Dr. Tessa Krantz answers common
Read MoreDr. Fagelson Named As A Center of Excellence for GreenLight Laser Therapy by Boston Scientific
Dr. James Fagelson designated as a Center of Excellence for GreenLight™ Laser Therapy, a Treatment for Benign Prostatic Hyperplasia (BPH), or Enlarged
Read MoreFact or Farce – Do Cranberries Cure Urinary Tract Infections?
When does the population consume more cranberries and drink more cranberry juice than during the holidays? For some who suffer from urinary
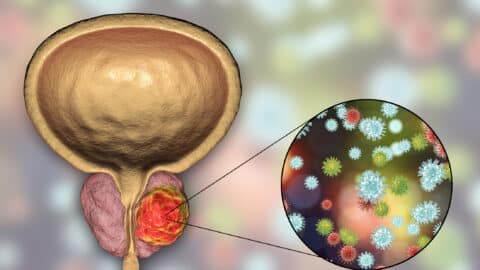
Read MoreThe Warning Signs of Prostate Cancer
Each year there are more than 30,000 prostate cancer deaths that could be prevented through prostate cancer screening, which helps to find prostate
Read MoreWhat Happens If Prostate Cancer Comes Back?
If prostate-specific antigen (PSA) levels remain high or become elevated after prostate cancer treatment, these are indications of a prostate
Read MoreHow Does Marijuana Affect Male Fertility?
The use of cannabis is on the rise, as it has become legal for both medical and recreational use in several states across the country.This comes with
Read MoreDa Vinci Prostatectomy Allowed Mark to Get Back To His Athletic Lifestyle!
Mark tells his story of a prostatectomy and traveling the road to recovery with the team at Urology Associates I want to give shout out
Read MoreCoping With CyberKnife Cancer Treatment Costs
A cancer diagnosis by itself is stressful and can be compounded by the financial burden incurred during cancer treatment. According to the American
Read MoreSeven Natural Ways to Prevent Kidney Stones
In some cases, a kidney stone diet may be enough to prevent stones from occurring and giving you kidney stone pain. While it is not complicated, it
Read MoreChanges in Bathroom Habits That Are Signs of Health Problems
Urologists and gynecologists, advises the importance of meeting with your primary care doctor if experiencing changes in bathroom habits. People often
Read MoreWhat Does Urine Color Say About Your Health?
Pay attention before you flush: know how to translate the message your urine color is sending you – especially if it is red, pink or brown. It
Read MoreWhat to Know Before Getting a Vasectomy
Dr. Brad Bell, along with other urologists, explained to AskMen what men should know before getting a vasectomy. Vasectomies are a readily available
Read MoreHis Successful Prostatectomy Proves All Urologists Are Not Equal
Our patient wrote this story about his life-changing treatment for BPH and elevated PSA with us, after he lost confidence in his previous
Read More